Foot Care for Diabetics
Proper foot care is essential for people with diabetes, as the skin is more sensitive and prone to friction wounds that can become serious.
Diabetics should visit a podiatrist regularly. Foot pulses and sensation should be checked frequently, as reduced sensation in the feet is common among those who have had diabetes for a long time. Circulation is also often impaired.
The foundation of diabetic foot care is to keep the feet soft and well-maintained to prevent cracks and wounds.
It is also possible to receive a doctor’s referral for foot care — KELA reimbursement may apply.
Book Your Appointment:
Medical Foot Care for Diabetics – 60 min
Comprehensive foot treatment tailored for diabetic patients, including nail and skin care, circulation check, and personalized guidance.
Diabetic Foot Assessment – 30 min
A focused examination of the condition of diabetic feet, including pulse measurement, sensation testing, and risk evaluation.

Self-Care for Diabetic Feet
- Check your feet daily.
- Look for wounds, cracks, redness, or any changes.
- Wash your feet regularly.
- Always dry carefully between the toes.
- Soak your feet occasionally.
- Use warm water (34–36°C) for a short foot bath.
- Always check the water temperature with a thermometer — never use water that’s too hot.
- Apply moisturizing cream to dry skin.
- Avoid applying cream between the toes.
- Trim your toenails regularly and straight across.
- If this is difficult, book an appointment with a podiatrist.
- Change your socks daily.
- Use cotton or wool socks without rubbing seams or tight elastic.
- Never walk barefoot.
- Wear comfortable indoor shoes and well-fitting footwear at all times.
- Always check your shoes before wearing them.
- Turn them upside down and remove any small stones or foreign objects.
- Never warm your feet directly on hot surfaces.
Why Professional Diabetic Foot Care Matters
Diabetes affects the body's ability to heal and fight infection. Over time, elevated blood sugar levels can lead to diabetic neuropathy — a condition that reduces sensation in the feet — and peripheral arterial disease, which limits blood flow to the lower extremities. Together, these complications mean that even minor injuries such as small cuts, blisters, or pressure sores can develop into serious infections or non-healing ulcers if left untreated.
Professional diabetic foot care goes beyond standard pedicure treatments. At ihoHUD in Vaasa, our trained specialists perform thorough assessments that include peripheral pulse measurement, monofilament sensation testing, and careful evaluation of skin integrity. These clinical checks help detect early warning signs of neuropathy and circulatory problems before they progress to more severe complications.
Regular professional foot care appointments also ensure that nails are trimmed correctly to prevent ingrown toenails, calluses and corns are safely reduced, and the skin barrier remains intact. Our podiatrists provide individualized guidance on daily foot care routines, appropriate footwear choices, and moisturizing techniques — all tailored to the unique needs of diabetic patients.
Early detection and consistent preventive care are the most effective ways to reduce the risk of diabetic foot complications. The Finnish Diabetes Association recommends that all diabetic patients have their feet examined by a healthcare professional at least once a year, with more frequent visits for those who have identified risk factors.
Related Foot Care Services
Frequently Asked Questions About Diabetic Foot Care
Diabetes can cause nerve damage (neuropathy) and poor circulation in the feet, which reduces the ability to feel pain and slows wound healing. Without proper foot care, minor injuries can go unnoticed and develop into serious infections or ulcers. In severe cases, untreated foot problems may lead to amputation. Regular professional foot care helps detect issues early and keeps the feet healthy.
At minimum, diabetic patients should have a comprehensive foot examination once a year. However, if you have neuropathy, poor circulation, a history of foot ulcers, or other risk factors, more frequent visits every 2–3 months are recommended. Your podiatrist will advise on the appropriate schedule based on your individual risk assessment.
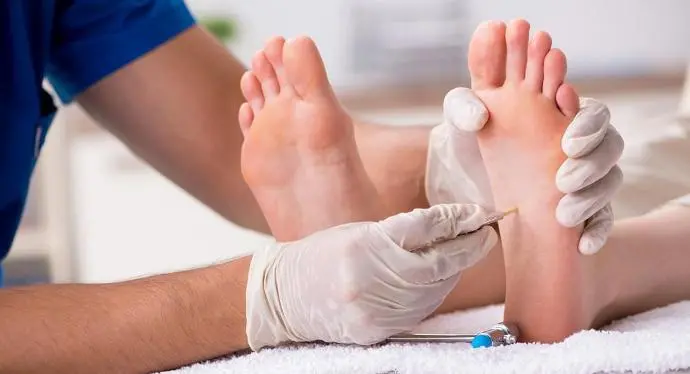
The monofilament test is a simple, painless clinical examination used to assess protective sensation in the feet. A thin, flexible nylon filament is pressed against specific points on the sole of the foot. If you cannot feel the filament, it indicates reduced sensation (peripheral neuropathy), which significantly increases the risk of unnoticed injuries. This test is a standard part of our diabetic foot assessment at ihoHUD.
Warning signs include tingling or numbness in the feet, cold or discoloured toes, slow-healing wounds or cuts, persistent redness or swelling, dry and cracking skin, thickened or discoloured nails, and pain or cramping in the calves when walking. If you notice any of these symptoms, schedule a professional foot assessment promptly. Early intervention is critical to preventing complications.
With a doctor's referral, diabetic foot care may qualify for partial KELA reimbursement in Finland. The referral should specify the medical necessity of podiatric treatment due to diabetes-related complications. We recommend consulting your treating physician about obtaining a referral, especially if you have documented neuropathy or circulatory issues. Our clinic can provide the necessary documentation for reimbursement claims.